Abstract
Aim The aims of the study were to assess the psychological impact of SARS bio-disaster on healthcare workers. Methods The participants were 127 healthcare workers who had taken care of suspected SARS patients. All participants completed the Chinese Health Questionnaire (CHQ), Eysenck Personality Questionnaire, and Parental Bonding Instrument at the first stage and the CHQ again a year later. Results Healthcare workers that had mental symptoms at follow-up reported the symptoms were associated with daily-life stress and not the SARS crisis. The physicians had more somatic symptoms than nurses, suggesting different professions have different impact on mental health. Additionally, individual’s early maternal attachment and neuroticism were found to have greater effect on mental health of life-threatening stress. Conclusions Life-threatening and daily-life stress show two different patterns of influence on mental health. These results provided a preclinical model for understanding, and preventing, human stress-related psychiatric disorders in the future.
Similar content being viewed by others
Introduction
After its first outbreak in Asia in February 2003, severe acute respiratory syndrome (SARS) quickly spread throughout several parts of the world. Over 8,000 people were affected by SARS, and an estimated 800 people died worldwide [1]. In March 2003, SARS broke out in Taiwan. Most of the survivors and aid personnel involved in the disaster experienced a stress reaction for several days or weeks [2]. Fear and anxiety usually appear immediately after the disaster and disappear within a short period of time, but the depression and psychophysical symptoms persist for a longer period of time [3]. If the psychological distress could be adjusted appropriately, the individual’s resilience and strength would be enhanced [4]. When healthcare workers were taking care of SARS patients, they not only had intense pressure from their workload, but also experienced stigma, fear, and frustration [5]. In fact, disasters decrease ones psychological well-being, and often appear in the form of depression [6].
Many studies have indicated that parental attachment influences the development of an individual’s personality [7–9], appropriate styles of coping [10], and psychological adjustment or mental health [7, 9, 11–13].These studies revealed that parental attachment and individual personality plays an important role in the individual’s stress coping ability and mental health.
The impact of this disaster on healthcare workers’ mental health has been studied; however, few follow-up investigations have been done. Thus, the aim of this study was to assess the psychological impact of the SARS bio-disaster on healthcare workers in diverse specialized fields by evaluating their mental health immediately after the SARS epidemic and again 1 year later, thereby gaining an understanding of the multiple pathways to the development of mental symptoms.
Methods
Participants
The study was a two-wave panel investigation. One-hundred and twenty-seven participants were recruited; these participants were divided into three groups based on the nature of their jobs, which served as a substitute for the level of exposure to SARS. These three groups are the physicians, the nurses, and the other healthcare workers (e.g., medical technicians, respiratory therapists, or emergency attendants). There were 24 male physicians, three male and 46 female nurses, and 26 male and 28 female other healthcare workers (Table 1). All of the participants responded to an initial mental health assessment between July 2003 and March 2004. During this period, the SARS epidemic was already under control after its main outbreak in April of 2003 [6]. Of the initial 127 participants, 123 participated in the follow-up investigation (96.9%) a year later.
Instruments
Parental Bonding Instrument (PBI)
Self-rated bonding behavior to parents has often been used as representative of parental attachment relationships [14–16].The PBI was developed by Parker et al. in 1979 [17]. Its Chinese version was written and revised in 1999 [18]. The PBI is a self-reported retrospective questionnaire which measures parental care and protection during childhood (before the age of 16). Subjects were asked to fill out two scales, one for each parent. There are 25 items in the questionnaire, and higher scores implicated higher care or protection. The Cronbach’s alpha ranges from 0.65 to 0.73, and the test–retest reliability ranges from 0.66 to 0.88 [18].
Eysenck Personality Questionnaire (EPQ)
The EPQ was developed based on Hans Eysenck’ theory of personality traits [19]. The Chinese version was developed by Lu in 1994 [20]. It is composed of two dimensions: 14 items for extraversion and 11 for neuroticism. Higher scores revealed higher levels of extraversion and neuroticism. The Cronbach’s alpha is 0.90, and good validity has been demonstrated [20].
Chinese Health Questionnaire (CHQ)
The CHQ is a 12 items self-administered screening instrument derived from the General Health Questionnaire, which is used to assess psychiatric morbidity [21]. Mental health status was dichotomized by an optimum cutoff point of 2/3 based on Receiver Operating Characteristic curves. The internal consistency resulted in Cronbach’s alpha of 0.79 [22]. The CHQ consisted of three dimensions: somatic symptoms, anxiety, and depression. However previous researches have revealed that negative affect was associated with somatic symptoms [23, 24] thus in the present study, anxiety and depression were merged, making two dimensions of somatic symptoms and negative affect (anxiety and depression).
Procedures
At the initial assessment, informed consent and demographics were collected from the participants. Additionally, they were asked to fill out the PBI, EPQ, and CHQ. At follow-up, a year after the initial assessment, the participants were asked to fill out the CHQ again, with an additional item asking the participants whether they have experienced any daily-life stressful event in the past year.
Statistical Analyses
Data were analyzed using the chi-square test, one-way ANOVA, and multiple linear regression using the SPSS 15.0 for Windows software package (SPSS, Chicago, IL). Only the parsimonious multiple linear regression results were presented in the current study, meaning only statistically significant variables were shown. The structural equation model (SEM) was analyzed using the AMOS 7.0 statistical software package. When the P value of the SEM was more than 0.05 and the adjusted sample size of goodness-of-fit index (AGFI) was more than 0.9, means that the observed data in the study were compatible with the null model and theoretical construct.
Results
Demographic and Psychosocial Characteristics
The demographics of the three groups (physicians, nurses, and other healthcare workers) are shown in Table 1. Among the 123 participants who were assessed at follow-up, 19 (15.4%) showed mental symptoms (CHQ ≧ 3), and 104 (84.6%) did not show obvious symptoms (χ2 = 2.14, P = 0.343). There was no significant difference in mental symptoms among the three groups (F = 2.11, P = 0.126). Additionally, 38 participants (30.9%) reported feelings of pressure from their life or job, and 85 (69.1%) had no significant daily-life stressful events during the follow-up period. No significant differences were found between the three groups in terms of feelings of stress (χ2 = 0.57, P = 0.752) (Table 1).
Multiple Linear Regression Analysis
Multiple linear regression analysis at both stages showed that there was no obvious relationship between participants’ mental health and other demographics, including age, gender, marital status, and occupation. At follow-up, educational level, the “paternal care” dimension of the PBI, neuroticism, and daily-life stressful events were predictors of mental symptoms. Lower education and higher neuroticism resulted in poorer mental health. Moreover, experience of daily-life stressful events during the year following the SARS attack had a negative impact on mental health (Table 2).
Structural Equation Model
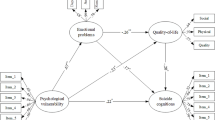
For the purpose of analysis, different combinations of participants were analyzed; the physicians (G1), nurses (G2), and other healthcare workers (G3) were regrouped into groups of twos (G1 and G2+3; G1+2 and G3; G2 and G1+3) since only 0–1 dichotomous dummy variables can be analyzed. These three different combinations were then placed in the model to test their relationships. In the initial assessment, the SEM showed that the combination of nurses versus physicians (G2 and G1+3) resulted in significant effect on participants’ mental health, thus this combination was adopted, as presented in Fig. 1a. Other than grouping, neuroticism, and maternal attachment affected the participants’ mental health status shortly after experiencing the SARS attack. Both maternal care and health profession influenced the participants’ mental symptoms negatively and directly (β = −0.18, P = 0.011; β = −0.14, P = 0.045). Additionally, maternal protection affected the participants’ neuroticism positively and directly (β = 0.36, P < 10−4), and neuroticism showed a positive and direct influence on mental symptoms (β = 0.54, P < 10−6), leading to maternal protection showing an indirect influence on the mental symptoms of participants shortly after experiencing the attack (β = 0.30, P < 10−4).
Robust parsimonious structural equation model of maternal attachment, neuroticism, and mental health for healthcare workers caring for SARS patients (nurses versus physicians and other healthcare workers). a Total CHQ scores. b Two dimensions (somatic symptoms and negative affect) of the CHQpbi_mc = maternal care; pbi_mp = maternal protection; epq_n = neuroticism; chq_t1 = total CHQ scores in the first stage; chq_t2 = total CHQ scores in the follow-up stage; somatic = somatic symptoms on the CHQ; NA, negative affect on the CHQ; event = daily-life stressful events. Dummy variables of group_n—1 refers to nurses, 0 refers to physicians combined with other healthcare workers
The dimension of maternal protection affected the participants’ neuroticism positively and directly (β = 0.36, P < 10−4), and neuroticism had a positive and direct impact on the participants’ mental symptoms at follow-up (β = 0.33, P < 10−4). Moreover, the experience of daily-life stressful event during the year after the SARS attack had a positive and direct impact on the participants’ mental symptoms (β = 0.29, P < 10−3). In other words, mental health would worsen for participants who were overprotected by their mother before age 16 when encountered with daily-life stressful events. There was no significant relationship between the initial and follow-up CHQ. Additionally under different stress conditions (life-threatening or daily-life stressful events), maternal attachment and neuroticism accounted for different amount in mental health variance. The SARS attack (life-threatening event) accounted for 38% of the variance in mental health, whereas daily-life stressful events accounted for 20% (Fig. 1a).
We further divided CHQ into the two dimensions of somatic symptoms and negative affect to examine their relationship with other variables (Fig. 1b). First, the first stage symptom results had a positive direct effect on the second stage results (somatic symptoms: β = 0.31, P < 10−4; negative affect: β = 0.23, P = 0.006). Second, the participants presented more somatic symptoms than negative affect at both stages (accounting for 35% and 19% of the variance, respectively), and the variance at the initial assessment accounted for almost twice the variance than at the follow-up assessment. Third, after classifying the mental symptoms at follow-up, maternal attachment or neuroticism had no causal influence on mental health. Daily-life stressful events had impact on both dimensions of mental health, which included somatic symptoms (β = 0.18, P = 0.034) and negative affect (β = 0.30, P < 10−4). Fourth, the major difference between the mental health of the nurses and the other healthcare workers was in the somatic realm (headache, palpitations, discomfort in the chest, and numbness of the limbs) in that the nurses had fewer complaints and symptoms (β = −0.15, P = 0.034). However, in the follow-up assessment, the nurses experienced somatic symptoms that were not significantly different from other healthcare workers. Fifth, participants who had negative affect at the initial assessment had fewer somatic symptoms (β = −0.21, P = 0.019) the following year. Last, negative affect had impact on somatic symptoms at both assessment stages (initial stage: β = 0.25, P < 10−4; follow-up stage: β = 0.24, P = 0.005). Individuals who had more negative affect reported more somatic complaints (Fig. 1b).
Discussion
In the initial assessment, 17.3% of the healthcare workers had mental symptoms shortly after the SARS epidemic was under control [9], and at one year follow-up, 15.4% of the participants had mental health symptoms. This proportion is less than the 24% estimated prevalence of psychiatric morbidity among the general population in Taiwan [21] and the 18.13% estimated prevalence in mainland China [25]. In the initial assessment, the stress was in response to the life-threatening SARS epidemic and in the follow-up assessment, from jobs, families, and daily-life stressful events and not from a continuation of previous symptoms, or vulnerability to or complications from stress created by the SARS attack. Maternal attachment and personality characteristics of neuroticism had a greater effect on life-threatening stress than daily-life stressful events since mental symptoms collected at the first stage (38%) accounted for almost twice the variance of second stage (20%) due to the differing nature and severity of the stress in the two stages (Fig. 1a).
Both stages of assessment revealed that negative affect can lead to somatic symptoms (Fig. 1b). This is consistent with the findings of Bailey and colleagues [23, 24]. In addition, in the first stage, with the stress from a serious life-threatening event, maternal attachment directly affected the development of the individual’s mental health, and in the second stage, with stress from daily life events, maternal attachment indirectly influenced the individual’s psychological health with personality characteristics being the mediator. Additionally, we found maternal and not paternal attachment. Stein and Call [26] pointed out that interpersonal trust is decided by a child’s attachment to the main caregiver during the critical period of 6 months to 3 years. The attachment system is activated when an individual is distressed or when there are threats in the environment guiding that person’s stress coping strategies [27]. Generally, the mother is the main caregiver during an individual’s infancy and childhood. Therefore, the relationship with the mother will mold his or her ability to adjust psychologically [7]. These are the possible reasons why, when faced with stress that threatens a person’s life, the way an individual responds to stress are influenced by early maternal attachment.
In terms of personality traits, the follow-up assessment found that after a traumatic experience, neurotic personality had an adverse effect on mental health, this is consistent with the results of the initial assessment. Thus, neuroticism was an important factor in influencing the individual’s mental health under different types of stresses. Previous investigations have indicated a strong test–retest correlation and stability of neurotic personality after 8 months [28], 1 year [29] and 10 years [30] follow-up, thus suggesting it is a stabilized characteristic. Moreover, studies have shown that neurotic personality was a predisposing factor for psychological distress [30, 31], and that the greater the disposition toward neuroticism, the easier it was to develop neurosis [31].
We also found that a higher percentage of physicians (35%), compared to nurses (25%), developed mental symptoms. This is consistent with the result of Chan and Huak [32] in Singapore. Furthermore, this study showed that during the SARS epidemic, the physicians presented more somatic complaints than the nurses (Fig. 1b). Aside from the stress of different jobs, the complaints could be related to socio-cultural and gender factors. In a different cultural dimension, Confucian dynamism has been used to explain some of the distinctive behavioral patterns in East Asian cultures, such as Taiwan, China, Hong Kong, Japan, and South Korea. One of the primary values of these cultures is the emphasis on the idea of “collective face-saving” [33]. In terms of the East Asian culture, men combine the characteristics of masculinity, assertiveness, and toughness with an emphasis on “saving face.” Because of this, men would feel embarrassed to show their soft side when confronted with stress. Therefore, most reactions would be physical (externalizing), with little display of anxiety or depression (internalizing). This corresponds with the research results of Gackenbach and Steer et al. [34, 35] who found that, compared with women, when in stressful situations men will have obvious physical symptoms, and seldom show emotions such as anxiety and hostility [34]. Women more frequently combine affective and cognitive symptoms in describing their depression, whereas men more frequently combine affective and performance symptoms [35]. In general, when coping with stress, Chinese tend to deny depression or express it somatically [36, 37]. Especially, men tend to have more frequent somatic complaints and anxiety, whereas most women tend to have more frequent social dysfunction [38]. However, this possible gender confounding factor was eliminated for both regression and SEM analysis showed that the impact of gender on mental health was minimal. Hence, the influence of occupation on mental health was greater than that of gender. Furthermore, physicians have higher educational levels than nurses; however, both the regression and SEM analysis results showed educational level did not have a statistically significant impact on mental health. Therefore, we hypothesize that the greater stress of physicians might be due to problems related to medical disputes and criminal law.
There were several limitations in this study. First, the current study used a self-descriptive inventory. Therefore, the mechanism of internal motivations is unknown. Further investigations of in-depth interviews or other objective assessments would provide more information to aid the development of more appropriate interventions. Second, subject grouping based on the level of exposure to SARS is difficult. Our study did not record the number of hours each participant worked, but we did group the participants based on their jobs. Third, this study did not measure the subjects’ mental health prior to the SARS outbreak; therefore we do not know if the post-SARS mental health might be attributable to pre-existing levels of mental health or the SARS crisis. Furthermore, we did not have a control group that did not have contact with SARS, making it difficult to know how much of the difference in mental health over time was related to the SARS outbreak versus some other variable. Future studies should collect initial and multiple measurements over time, and analyze the data using latent growth curve models to calculate the inter-individual differences in change over time [39]. Despite these limitations, the present study demonstrated the immediate effect of the SARS outbreak, and the changes that occurred after 1 year in terms of factors that impacted the mental health of healthcare workers.
The results of this study suggest that parental attachment, personality, and mental health showed two different patterns of influence from life-threatening and daily-life stressful events. Additionally, maternal attachment and neuroticism significantly influenced the mental health of those caring for SARS patients. Moreover, different professions were associated with different psychiatric symptoms. An individual’s negative affect may lead to somatic symptoms. This study provided a preclinical model for improving our understanding, and developing prevention programs for stress-related psychiatric disorders in the future.
References
Hussein A: SARS—future considerations for nurses. Journal of Advanced Nursing 45:111–112, 2004. doi:10.1111/j.1365-2648.2004.02907.x
Lan P: Stress management: A total approach. Taipei, Taiwan, Youth Culture Company, 2003
Shioyama A, Uemoto M, Shinfuku N, et al.: The mental health of school children after the Great Hanshin-Awaji Earthquake: II. Longitudinal analysis. Seishin Shinkeigaku Zasshi 102:481-497, 2000
Reacher M, McKenzie K, Lane C, et al.: Health impacts of flooding in Lewes: A comparison of reported gastrointestinal and other illness and mental health in flooded and non-flooded households. Communicable Disease and Public Health 7:39–46, 2004
Robertson E, Hershenfield K, Grace SL, et al.: The psychosocial effects of being quarantined following exposure to SARS: A qualitative study of Toronto health care workers. Canadian Journal of Psychiatry 49:403–407, 2004
Adams RE, Boscarino JA: Differences in mental health outcomes among Whites, African Americans, and Hispanics following a community disaster. Psychiatry 68:250–265, 2005. doi:10.1521/psyc.2005.68.3.250
Punamaki RL, Qouta S, el Sarraj E: Models of traumatic experiences and children’s psychological adjustment: The roles of perceived parenting and the children’s own resources and activity. Child Development 68:718–728, 1997. doi:10.2307/1132121
Lung FW, Lee FY, Shu BC: The relationship between life adjustment and parental bonding in military personnel with adjustment disorder in Taiwan. Military Medicine 167:678–682, 2002
Lu YC, Shu BC, Chang YY, et al.: The mental health of hospital workers dealing with severe acute respiratory syndrome. Psychotherapy and Psychosomatics 75:370–375, 2006. doi:10.1159/000095443
Matheson K, Kelly O, Cole B, et al.: Parental bonding and depressive affect: The mediating role of coping resources. The British Psychological Society 44:371–395, 2005. doi:10.1348/014466605X37477
Perris C, Jacobsson L, Lindstrom H, et al.: Development of a new inventory assessing memories of parental rearing behaviour. Acta Psychiatrica Scandinavica 61:265–274, 1980. doi:10.1111/j.1600-0447.1980.tb00581.x
Sroufe LA: Infant-caregiver attachment and patterns of adaptation in preschool: The roots of maladaptation and competence. In: Perlmutter M (Ed) Minnesota Symposium in Child Psychology, Vol. 16, Hillsdale, New Jersey, Lawrence Erlbaum Associates, 1983
Maccoby EE: The role of parents in the socialization of children: a historical overview. Developmental Psychology 28:1006–1017, 1992. doi:10.1037/0012-1649.28.6.1006
Gilbert P, Gerlsma C: Recall of shame and favouritism in relation to psychopathology. The British Journal of Clinical Psychology 38:357–373, 1999. doi:10.1348/014466599162962
Rankin P, Bentall R, Hill J, et al.: Perceived relationships with parents and paranoid delusions: Comparisons of currently III, remitted and normal participants. Psychopathology 38:16–26, 2005. doi:10.1159/000083966
Willinger U, Diendorfer-Radner G, Willnauer R, et al.: Parenting stress and parental bonding. Behavioral Medicine 31:63–69, 2005. doi:10.3200/BMED.31.2.63-72
Parker G, Tupling H, Brown LE: A parental bonding instrument. The British Journal of Medical Psychology 52:1–10, 1979
Shu BC, Lo WJ, Lung FW: The reliability and validity of a Chinese version of the Parental Bonding Instrument. Nursing Research 7:479–489, 1999
Eysenck HJ, Eysenck SBG: Manual for the Eysenck Personality Questionnaire. London, Hodder & Stoughton, 1975
Lu L: University transition: Major and minor life stressors, personality characteristics and mental health. Psychological Medicine 24:81–87, 1994
Cheng TA, Williams P: The design and development of a screening questionnaire (CHQ) for use in community studies of mental disorders in Taiwan. Psychological Medicine 16:415–422, 1986
Cheng TA, Wu JT, Chong MY, et al.: Internal consistency and factor structure of the Chinese Health Questionnaire. Acta Psychiatrica Scandinavica 82:304–308, 1990. doi:10.1111/j.1600-0447.1990.tb01389.x
Bailey PE, Henry JD: Alexithymia, somatization and negative affect in a community sample. Psychiatry Research 150:13–20, 2007. doi:10.1016/j.psychres.2006.05.024
Lundh LG, Simonsson-Sarnecki M: Alexithymia, emotion, and somatic complaints. Journal of Personality 69:483–510, 2001. doi:10.1111/1467-6494.00153
Yang TZ, Huang L, Wu ZY: The application of Chinese Health Questionnaire for mental disorder screening in community settings in mainland China. Zhonghua Liu Xing Bing Xue Za Zhi 24:769–773, 2003
Stein MT, Call JD: Extraordinary changes in behavior in an infant after a brief separation. Journal of Developmental and Behavioral Pediatrics 22:11–15, 2001
Rutgers AH, Bakermans-Kranenburg MJ, van IJzendoorn MH, et al.: Autism and attachment: A meta-analytic review. Journal of Child Psychology and Psychiatry 45:1123–1134, 2004. doi:10.1111/j.1469-7610.2004.t01-1-00305.x
Cramer D: Psychological distress and neuroticism: A two-wave panel study. The British Journal of Medical Psychology 67:333–342, 1994
Simon A, Thomas A: Means, standard deviations and stability coefficients on the EPI for further education and college of education students. Personality and Individual Differences 4:95–96, 1983. doi:10.1016/0191-8869(83)90056-9
Ormel J, Wohlfarth T: How neuroticism, long-term difficulties, and life situation change influence psychological distress: A longitudinal model. Journal of Personality and Social Psychology 60:744–755, 1991. doi:10.1037/0022-3514.60.5.744
Eysenck HJ, Eysenck MW: Personality and individual differences: A natural science approach. New York and London, Plenum Press, 1985
Chan AO, Huak CY: Psychological impact of the 2003 severe acute respiratory syndrome outbreak on health care workers in a medium size regional general hospital in Singapore. Occupational Medicine 54:190–196, 2004. doi:10.1093/occmed/kqh027
Ting-Toomey S: Value orientations and intercultural encounters. In: Glasser TL, Poole MS (Eds) Communicating across cultures. New York, Guilford Press, 1999
Gackenbach J: Collegiate swimmers: Sex differences in self-reports and indices of physiological stress. Perceptual and Motor Skills 55:555–558, 1982
Steer RA, Beck AT, Brown G: Sex differences on the revised beck depression inventory for outpatients with affective disorders. Journal of Personality Assessment 53:693–702, 1989. doi:10.1207/s15327752jpa5304_6
Kleinman AM: Depression, somatization and the new cross-cultural psychiatry. Social Science & Medicine 11:3–10, 1977. doi:10.1016/0037-7856(77)90138-X
Parker G, Gladstone G, Chee KT: Depression in the planet’s largest ethnic group: The Chinese. The American Journal of Psychiatry 158:857–864, 2001
Tang CS, Lau BH: The Chinese gender role stress scales. Factor structure and predictive validity. Behavior Modification 20:321–337, 1996. doi:10.1177/01454455960203005
Willett JB, Sayer AG: Using covariance structure analysis to detect correlates and predictors of individual change over time. Psychological Bulletin 116:363–381, 1994. doi:10.1037/0033-2909.116.2.363
Acknowledgments
This research was supported by a grant (NSC93-2625-Z-393-001) from the National Science Council, Executive Yuan, Taiwan. The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lung, FW., Lu, YC., Chang, YY. et al. Mental Symptoms in Different Health Professionals During the SARS Attack: A Follow-up Study. Psychiatr Q 80, 107–116 (2009). https://doi.org/10.1007/s11126-009-9095-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11126-009-9095-5