Abstract
OBJECTIVES: To compare statin nonadherence and discontinuation rates of primary and secondary prevention populations and to identify factors that may affect those suboptimal medication-taking behaviors.
DESIGN: Retrospective cohort utilizing pharmacy claims and administrative databases.
SETTING: A midwestern U.S. university-affiliated hospital and managed care organization (MCO).
PATIENTS: Non-Medicaid MCO enrollees, 18 years old and older, who filled 2 or more statin prescriptions from January 1998 to November 2001; 2,258 secondary and 2,544 primary prevention patients were identified.
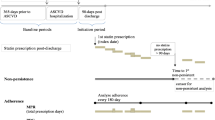
MEASUREMENTS: Nonadherence was assessed by the percent of days without medication (gap) over days of active statin use, a measurement known as cumulative multiple refill-interval gap (CMG). Discontinuation was identified by cessation of statin refills prior to the end of available pharmacy claims data.
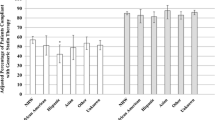
RESULTS: On average, the primary and secondary groups went without medication 20.4% and 21.5% of the time, respectively (P=.149). Primary prevention patients were more likely to discontinue statin therapy relative to the secondary prevention cohort (relative risk [RR], 1.24; 95% confidence interval [CI], 1.08 to 1.43). Several factors influenced nonadherence and discontinuation. Fifty percent of patients whose average monthly statin copayment was <$10 discontinued by the end of follow-up (3.9 years), whereas 50% of those who paid >$10 but ≤$20 and >$20 discontinued by 2.2 and 1.0 years, respectively (RR, 1.39 and 4.30 relative to <$10 copay, respectively).
CONCLUSIONS: Statin nonadherence and discontinuation was suboptimal and similar across prevention categories. Incremental efforts, including those that decrease out-of-pocket pharmaceutical expenditures, should focus on improving adherence in high-risk populations most likely to benefit from statin use.
Similar content being viewed by others
References
Shepherd J, Cobe SM, Ford I, et al. Prevention of coronary heart disease with pravastatin in men with hypercholesterolemia: West of Scotland Coronary Prevention Study Group. N Engl J Med. 1995;333:1301–7.
Bradford RH, Shear CL, Chremos AN, et al. Expanded Clinical Evaluation of Lovastatin (EXCEL) study result. I. Efficacy in modifying plasma lipoproteins and adverse event profile in 8245 patients with moderate hypercholesterolemia. Arch Intern Med. 1991;151:43–9.
Downs JR, Clearfield M, Weis S, et al. Primary prevention of acute coronary events with lovastatin in men and women with average cholesterol levels: results of ASCAPS/TexCAPS. JAMA. 1998;279:1615–22.
Scandinavian Simvastatin Survival Study Group. Randomized trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S). Lancet. 1994;344:1383–9.
The LIPID Study Group. Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. N Engl J Med. 1998;339:1349–57.
Sacks FM, Pfeffer MA, Moye LA, et al. The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. N Engl J Med. 1996;335:1001–9.
Kumana CR, Cheung B, Lauder IJ. Gauging the impact of statins using number needed to treat. JAMA. 1999;282:1899–901.
McDermott MM, Schmitt B, Wallner E. Impact of medication non-adherence on coronary heart outcomes: a critical review. Arch Intern Med. 1997;157:1921–9.
Mäenpää H, Heinonen OP, Manninen V. Medication compliance and serum lipid changes in the Helsinki Heart Study. Br J Clin Pharmacol. 1991;32:409–15.
The West of Scotland Coronary Prevention Study Group. Compliance and adverse event withdrawal: their impact on the West of Scotland Coronary Prevention Study. Eur Heart J. 1997;18:1718–24.
Andrade SE, Walker AM, Gottleib LK, et al. Discontinuation of antihyperlipidemic drugs—do rates reported in clinical trials reflect rates in primary care settings? N Engl J Med. 1995;332:1125–31.
Avorn J, Monette J, Lacour A, et al. Persistence of use of lipid-lowering medications: a cross-national study. JAMA. 1998;279:1458–62.
Sung JCY, Nichol MB, Venturini F, Bailey KL, McCombs JS, Cody M. Factors affecting patient compliance with antihyperlipidemic medications in an HMO population. Am J Manag Care. 1998;4:1421–30.
Benner JS, Glynn RJ, Mogun H, Neumann PJ, Weinstein MC, Avorn J. Long-term persistence in use of statin therapy in elderly patients. JAMA. 2002;288:455–61.
Jackevicius CA, Mamdani M, Tu JV. Adherence with statin therapy in elderly patients with and without acute coronary syndromes. JAMA. 2002;288:462–7.
Taylor H, Leitman R. Out-of-pocket costs are a substantial barrier to prescription drug compliance. Health Care News. November 20, 2001.
Reed-Haldy-McIntosh for AARP. Prescription Drug Use Among Persons Age 45+. Survey; April 2002.
Cunningham PJ. Affording Prescription Drugs: Not Just a Problem for the Elderly. Center for Studying Health System Change. Washington, DC: Research Report No. 5; April 2002.
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of the Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA. 2001;285:2486–97.
Health Plan Employer Data and Information Set (HEDIS). Cholesterol Management After Acute Cardiovascular Events. Washington, DC: National Committee for Quality Assurance; 2002.
Steiner JF, Koepsell TD, Fihn SD, Inui TS. A general method of compliance assessment using centralized pharmacy records: description and validation. Med Care. 1988;26:814–23.
Steiner JF, Prochazka AV. The assessment of refill compliance using pharmacy records: methods, validity, and applications. J Clin Epidemiol. 1997;50:105–16.
Heeschen C, Hamm CW, Laufs U, et al. Withdrawal of statins increases event rates in patients with acute coronary syndromes. Circulation. 2002;105:1446–52.
Thomas M, Mann J. Increased thrombotic vascular events after change of statin. Lancet. 1998;352:1830–1.
White TJ, Chang E, Leslie S, et al. Patient adherence with HMG reductase inhibitor therapy among users of two types of prescription services. J Manag Care Pharm. 2002;8:186–91.
Wei L, Wang J, Thompson P, Wong S, Struthers AD, MacDonald TM. Adherence to statin treatment and readmission of patients after myocardial infarction: a six year follow-up study. Heart. 2002;88:229–33.
Joyce GF, Escarce JJ, Solomon MD, Goldman DP. Employer drug benefit plans and spending on prescription drugs. JAMA 2002;288:1733–9.
Motheral BR, Henderson R. The effect of a copay increase on pharmaceutical utilization, expenditures, and treatment continuation. Am J Manag Care. 1999;5:1383–94.
Fendrick AM, Smith DG, Chernew ME, Shaw SN. A benefit-based copay for prescription drugs: patient contribution based on total benefits, not drug acquisition cost. Am J Manag Care. 2001;7:861–7.
Nelson K, Norris K, Mangione CM. Disparities in the diagnosis and pharmacologic treatment of high serum cholesterol by race and ethnicity. Arch Intern Med. 2002;162:929–35.
Salganicoff A, Beckman JZ, Wyn R, Ojeda VD. Women’s Health in the United States: Health Coverage and Access to Care. Report by The Henry J. Kaiser Foundation; May 2002.
Claxton AJ, Cramer J, Pierce C. A systematic review of the associations between dose regimens and medication compliance. Clin Ther. 2001;23:1296–10.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ellis, J.J., Erickson, S.R., Stevenson, J.G. et al. Suboptimal statin adherence and discontinuation in primary and secondary prevention populations. J GEN INTERN MED 19, 638–645 (2004). https://doi.org/10.1111/j.1525-1497.2004.30516.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2004.30516.x